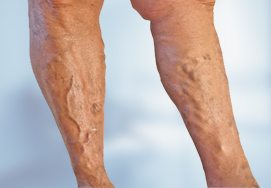
Varicose Veins
Varicose veins are red or blue coloured veins that one can observe under the skin. Besides being a cosmetic problem, varicose veins can be painful, especially when standing.
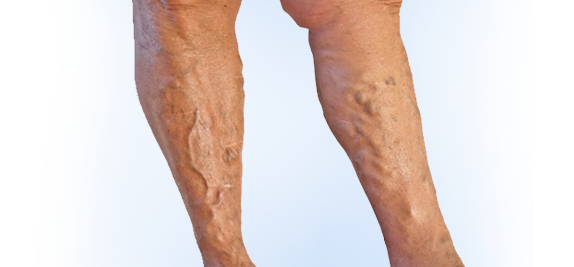
- what are varicose veins ?
- What are the symptoms of varicose veins ?
- What are the causes of varicose veins?
- How is varicose veins classified?
- What are the complications of varicose veins?
- What are the treatment options?
-
How does the endovenous thermal ablation
work? -
How is endovenous thermal ablation
procedure performed? -
What are the risks and benefits of
Endovenous ablation -
What are the limitations of Endovenous
Ablation of Varicose Veins? - What is secondary varicose vein?
what are varicose veins ?
Varicose veins are swollen, twisted, and enlarged veins that you can see under the skin. They are often red or blue in colour. They usually appear in the legs, but can occur in other parts of the body. Besides being a cosmetic problem, varicose veins can be painful, especially when standing. Severe long-standing varicose veins can lead to leg swelling, venous eczema, skin thickening (lipodermatosclerosis) and ulceration.
What are the symptoms of varicose veins ?
- Visible, swollen veins
- Aching, heavy legs (often worse at night and after exercise).
- Appearance of spider veins (telangiectasia) in the affected leg.
- Ankle swelling, especially in the evening.
- A brownish-yellow shiny skin discoloration near the affected veins.
- Redness, dryness, and itchiness of areas of skin, termed stasis dermatitis or venous eczema, because of waste products building up in the leg.
- Cramps may develop especially when making a sudden move as standing up.
- Minor injuries to the area may bleed more than normal or take a long time to heal.
- In some people the skin above the ankle may shrink (lipodermatosclerosis) because the fat underneath the skin becomes hard.
- Restless legs syndrome appears to be a common overlapping clinical syndrome in patients with varicose veins and other chronic venous insufficiency.
- Whitened, irregular scar-like patches can appear at the ankles. This is known as atrophie blanche.
What are the causes of varicose veins?
Normally, one-way valves in your leg veins keep blood moving up toward the heart. When the valves do not work properly, they allow blood to back up into the vein. The vein swells from the blood that collects there, which causes varicose veins. Smaller varicose veins that you can see on the surface of the skin are called spider veins.
Varicose veins are more common in women than in men, and are linked with heredity. Other risk factors are
- Older age
- Pregnancy,
- Obesity,
- Menopause, Aging,
- Prolonged Standing,
- Leg Injury
- and Abdominal Straining.
- chronic alcohol consumption
How is varicose veins classified?
According to the CEAP (Clinical, Etiological, Anatomical and Pathological ) classification
Clinical
- C0 –no visible or palpable signs of venous disease
- C1 – telangectasia or reticular veins
- C2 –varicose veins.
- C3 –edema
- C4a –pigmentation or eczema
- C4b –lipodermatosclerosis, atrophie blanche
- C5 –healed venous ulcer
- C6 –active venous ulcer •Each clinical class is further characterised by a subscript depending upon whether the patient is symptomatic (S) or asymptomatic (A)
S = Symptomatic, including ache, pain, tightness, skin irritation, heaviness, and muscle cramps, and other complaints attributable to venous dysfunction A = Asymptomatic
| Etiological classification | Anatomical classification | Pathophysiology |
| Ec: congenital | As: superficial veins | Pr: reflux |
| Ep: primary | Ap: perforating veins | Po: obstruction |
| Es: secondary | Ad: deep veins | Pr,o: reflux and obstruction |
| En: no venous cause identified | An: no venous location identified | Pn: no venous pathophysiology identifiable |
What are the complications of varicose veins?
Most varicose veins are reasonably benign, but severe varicosities can lead to major complications, due to the poor circulation through the affected limb.
- Pain, tenderness, heaviness, inability to walk or stand for long hours, thus hindering work
- Skin conditions / Dermatitis which could predispose skin loss
- Skin ulcers especially near the ankle, usually referred to as venous ulcers.
- Development of carcinoma or sarcoma in longstanding venous ulcers. Over 100 reported cases of malignant transformation have been reported at a rate reported as 0.4% to 1%.[7]
- Severe bleeding from minor trauma, of particular concern in the elderly.
- Blood clotting within affected veins, termed superficial thrombophlebitis. These are frequently isolated to the superficial veins, but can extend into deep veins, becoming a more serious problem.
- Acute fat necrosis can occur, especially at the ankle of overweight patients with varicose veins. Females are more frequently affected than males.
What are the treatment options?
The National Institute for Health and Clinical Excellence (NICE) produced clinical guidelines in July 2013 recommending that all people with symptomatic varicose veins (C2S) and worse should be referred for surgical treatment. Conservative treatments such as support stockings should not be used unless definitive treatment was not possible
Conservative
The symptoms of varicose veins can be controlled to an extent with the following:Elevating the legs often provides temporary symptomatic relief.
- Do not sit or stand for long periods. Even moving your legs slightly helps keep the blood flowing.
- Elevating the legs often provides temporary symptomatic relief.Raise your legs above your heart three or four times a day for 15 minutes at a time.
- Wearing of graduated compression stockings with variable pressure gradients (Class II or III) has been shown to correct the swelling, nutritional exchange, and improve the microcirculation in legs affected by varicose veins. They also often provide relief from the discomfort associated with this disease.
- Wearing of intermittent pneumatic compression devices have been shown to reduce swelling and increase circulation
- Lose weight if you are overweight.
Surgical treatment
As most of the blood in the legs is returned by the deep veins, the superficial veins, which return only about 10% of the total blood of the legs, can usually be removed or ablated without serious harm
Surgical treatment is recommended when there is failure of conservative treatment and worsening of symptoms.
- Stripping – traditionally varicose veins were stripped
Requires surgical incisions along with ligation and stripping of the vein. Scars are visible and down time is slightly longer. - Endovenous thermalablationuses radiofrequency or laser energy to cauterize and close varicose veins in the legs. It may be used for cosmetic purposes, but it is most commonly used to help alleviate related symptoms such as aching, swelling, skin irritation, discoloration or inflammation. Endovenous ablation is safe, less invasive than conventional surgery, and leaves virtually no scars
How does the endovenous thermal ablation work?
Ultrasound is used to visualize the varicose vein. A laser fiber or radiofrequency electrode is advanced to the desired location within the vein. Laser or radiofrequency energy is then applied, heating the vessel and causing it to close. Following the procedure, the faulty vein will shrink and “scar down.”
How is endovenous thermal ablation procedure performed?
This procedure is often done on an outpatient basis. However, some patients may require admission following the procedure. Please consult with your surgeon as to whether or not you will be admitted.
Your surgeon may use a topical anesthetic cream over the abnormal vein area before the procedure in order to reduce discomfort.
The leg being treated will be cleaned, sterilized and covered with a surgical drape.
Your physician will numb the area where the catheter will enter into the abnormal vein with a local anesthetic and use the ultrasound transducer or wand to study the vein and track its path.
A very small skin incision is made at the site.
Using ultrasound guidance, a catheter or vascular access sheath is inserted through the skin and positioned within the abnormal vein. The laser fiber or radiofrequency electrode is inserted through the catheter and the tip of the fiber or electrode is exposed by pulling the catheter back slightly.
Local anesthetic is injected around the abnormal vein with ultrasound guidance. Laser or radiofrequency energy is applied as the catheter is slowly withdrawn.
Pressure will be applied to prevent any bleeding and the opening in the skin is covered with a bandage. No sutures are needed.
This procedure is usually completed within an hour.
What are the risks and benefits of Endovenous ablation
Benefits
- No surgical incision is needed—only a small nick in the skin that does not have to be stitched.
- When compared with traditional vein stripping techniques, endovenous ablation is more effective, has fewer complications, and is associated with much less pain during recovery.
- Endovenous ablation is generally complication-free and safe.
- This procedure leaves virtually no scars because catheter placement requires skin openings of only a few millimeters, not large incisions.
- Endovenous ablation offers a less invasive alternative to standard surgery.
- Most of the veins treated are effectively invisible even to ultrasound 12 months after the procedure.
- Most patients report symptom relief and are able to return to normal daily activities immediately, with little or no pain.
Risks
- Any procedure where the skin is penetrated carries a risk of infection. The chance of infection requiring antibiotic treatment appears to be less than one in 1,000.
- Any procedure that involves placement of a catheter inside a blood vessel carries certain risks. These risks include damage to the blood vessel, bruising or bleeding at the puncture site, and infection.
- Some post-procedure bruising and tenderness may occur, but may be alleviated by wearing a compression stocking.
- Some instances of thermal (heat) damage to nerves have been reported. This is rare and generally goes away in a short time.
- Thrombophlebitis (inflammation of the vein) is not uncommon and may cause pain and redness over the treated area, but generally responds well to nonsteroidial anti-inflammatory drugs (NSAIDs).
- Blood clots that formed in the veins can travel to the lungs (pulmonary embolism); however, this is an extremely rare occurrence.
What are the limitations of Endovenous Ablation of Varicose Veins?
- Ablation catheters cannot be easily passed through a vessel with many turns and bends (tortuous vein). Consequently, endovenous ablation is typically used to treat larger varicose veins, such as the great saphenous vein, which extends from the groin and inside of the thigh into the inner calf.
- Endovenous ablation is successful at closing the abnormal target vein almost 100 percent of the time, but small dilated branches that persist in the skin often require additional treatment with phlebectomy (minor surgical procedure to extract them) or sclerotherapy (injection of a liquid medication to seal them off). Subsequent treatments are usually scheduled after an ablation procedure
What is secondary varicose vein?
Secondary varicose veins are those developing as collateral pathways, typically after stenosis or occlusion of the deep veins, a common sequel of extensivedeep venous thrombosis(DVT). Treatment options are usually support stockings, occasionally sclerotherapy and rarely, limited surgery.