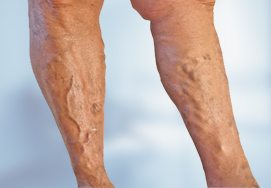
Diabetic Foot Salvage And Reconstruction
Indicated in diabetic patients

- What is diabetic foot surgery?
- What are the types of the surgeries?
- Which individuals are suitable for the surgery?
- How should I prepare for the surgery?
- What will happen during the surgery?
- What is the aftercare of the surgery?
- What are the postsurgical considerations?
What is diabetic foot surgery?
Diabetic foot ulcers occur in nearly 15% of people with diabetes mellitus. Diabetes affects nerves in the foot and alters the blood flow that develops over time and prevents injuries from healing. Even a minor injury can become a major infection in these patients, and hence it is very important to keep the foot healthy in diabetics.
The symptoms of the diabetic foot problems include pain and tingling sensation in the feet (especially at night), unsteadiness in standing, and walking due to lack of sensation. Swelling of the foot, redness, ulcers and bleeding are seen in severe stages. Some ulcers may be painless due to presence of neuropathy. Therefore, diabetic patients should have self-inspection of each foot regularly.
Most of the non-infected foot ulcers can be treatable without surgery using antibiotics. However, surgery is required in some patients to remove pressure on the affected area including excision of bones, correct the deformities such as bunions or bony “bumps”, and to treat infections of the bone.
The main aim of surgical therapy for diabetic foot ulcer is to control the deep infection, which can be accomplished by draining the pus, removing the infected tissues and creating a healthy wound bed. And then the aim is to cover the wound with soft tissue to attain stable soft tissue coverage so as to achieve early wound healing and prevent the ulcer from being reinfected
Diabetic foot management requires in-depth knowledge of the anatomy of the foot , and should be done by none other than plastic surgeons who are trained in both reconstruction and microsurgery. Knowledge in reconstruction and microsurgery helps in taking good decisions.
What are the types of the surgeries?
Surgical procedures range from simple outpatient debridements to amputations in patients with life-threatening infections. There are various surgical options which are considered by the surgeons depending on the patient’s condition.
Debridement
This is the mainstay of treatment in diabetics. It should be done properly and should not be regarded as a simple procedure. Otherwise the infection can flare up after a poorly done debridement. It involves debridement of nonviable and infected tissue from the ulceration. The diabetic patient usually requires surgical debridement to determine the depth and involvement of bone structures.
Vascular reconstruction
Vascular surgery in the presence of a reconstructible arterial lesion is required for patients with uncontrollable pain at night, uncontrollable foot ulcers and existing gangrene.
Skin grafting
This is done to cover the wounds and make them heal fast without which ulcer will not heal and is likely to get reinfected.
Microvascular free tissue transfers
These are done to save the foot and provide stable coverage in severe diabetic foot infections.
Which individuals are suitable for the surgery?
Most diabetic patients with diabetic foot are suitable for surgery. Milder infections can be managed with antibiotics. But anything more requires timely management as neglecting the initial infection can make it flare up and result in larger problem.
Never neglect an infection with diabetes. Take specialist opinion to prevent major infection
How should I prepare for the surgery?
- Diabetic foot surgery is performed effectively only when performed by qualified specialists
- Before the surgery, the surgeon considers the vascular status of the affected limb and the anatomic status at which the wound would be likely to heal. The surgeon also ensures that there is sufficient soft tissue to cover the deficits left by the resections or amputation.
Complete pre-operative tests should be done and assessed effectively prior to the surgery.
- You should arrange someone to drive back home and to stay with you in the hospital after the surgery.
- You should stop taking medications like aspirin and other non-steroidal anti-inflammatory drugs prior to the surgery to prevent bleeding.
- You should take the medications as suggested by your surgeon.
- Before the surgery, the surgeon may recommend few exercises to strengthen the upper body to prepare for crutch or walker use after the surgery.
What will happen during the surgery?
Any diabetic foot surgery should consist of at least two settings , but can be more if infection is still persisting.
First – clearance of infection
Intermediate stage – negative pressure wound therapy
Second – coverage of resultant wound to provide stable coverage
At first, the patient will be given anesthesia, local or general depending on the patient’s condition. The surgical management of diabetic foot infections is done in various steps. In the first step, the surgeon makes an incision in the wound area starting with the distal most area of the infection and extending to the proximal area. Then the surgeon investigates the wound to determine the size and extent of soft tissue involvement and the presence of foreign bodies, abscess, or sinus tracts. Then the surgeon debrides all the non-viable tissue and bone and exposed tendons to reduce the spread of infection. Then the surgeon cleanses the wound using saline or antibiotic solution to reduce the incidence of continued infection. After eliminating the infected diabetic foot wound, the wound is closed.
Intermediately – you may require to undergo negative pressure wound therapy to reduce infection. And provide for drainage of the wound and promote granulation tissue which resists infection by forming a barrier..
Second stage – Your wound will be covered with either a skin graft in simple cases or if required a microvascular free flap coverge to salvage a foot in complicated cases.
What is the aftercare of the surgery?
Healing should take less than a month.
You may experience numbness tingling, and burning sensation in the surgical site soon after the surgery. You should elevate your foot above the heart for 48 hours after the surgery. This helps in relieving pain and sensations. If the pain still persists, you can call the surgeon immediately because it may be due to the cast or tight dressing.
You should follow the surgeon’s instructions carefully for easy and quick recovery.
- Avoid prolonged sitting or standing and putting weight on the surgical area.
- Will have to walk with on Microcellular rubber (MCR) chappals/ shoes but not bare foot
- Foot wear should be soft and should be changed regularly
- You will have to inspect the foot regularly
- Take pain medications as prescribed by your surgeon. They may cause nausea or constipation, so, take fiber rich food.
- The surgical dressings placed at the time of surgery will be left intact until your first postoperative visit.
What are the postsurgical considerations?
- Avoid walking barefoot at all times
- Inspect foot carefully every day for any injuries or infection
- Use soft padded chappals or shoes.
- Change your foot wear regularly.