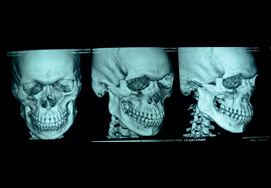
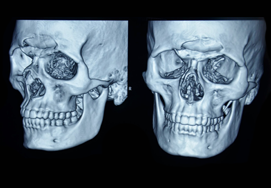
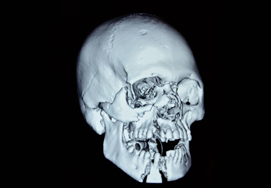
Maxillary Fracture
Performed in individuals with difficulty in opening mouth, ecchymosis (discoloration of the skin), trauma, and problem in the vision
- What is a maxillary fracture?
- What are the types of maxillary fractures?
- What are the types of surgeries?
- Which individuals are eligible for the surgery?
- How should I prepare for the surgery?
- What will happen during the surgery?
- What is the aftercare of the surgery?
- What are the postsurgical considerations?
What is a maxillary fracture?
The maxilla is a combination of two bones that forms the upper jawbone. Maxillary fractures usually occur when the front of the face smashes against an immovable object, or during a fall from a height or motor vehicle accident and after a dental or medical procedure. Maxillary fractures often cause swelling and deformity of the face. Other symptoms depend on the severity of the fracture. It may cause double vision, numbness of the skin below the eyes, inability to fully open the jaw, injury to the spine in the neck and sometimes brain injury. This occurs if the fracture involves other parts of the face.
What are the types of maxillary fractures?
A fracture of the maxilla occurs less frequently compared to mandible or nose as the maxilla has strong structural support. The maxilla provides protection for the brain, projection of the mid-face and supports for occlusion (blockage of blood vessel). There are three types of maxillary fractures;
The LeFort I fracture, also called transverse fracture extends through the base of the maxillary sinuses above the teeth separating the alveolar processes, palate, and pterygoid processes from the facial structures above. The fracture across the entire maxilla separates the alveolus from the rest of the midface. In the case of severe injuries, the palate may be split in the midline including LeFort I fracture.
The LeFort II fracture or pyramidal fracture is similar to LeFort I fracture, but medially diverges to include part of the medical orbit as well as the nose. The fracture across the nose may involve only the nasal cartilage or separate the nasofrontal structure. From pterygoid plates, the fracture extends diagonally through the maxilla to the inferior orbital rim, up the medial wall of the orbit to the nose. Due to this the maxillary alveolus, a medical wall of the orbit and nose are separated.
In LeFort III fracture or craniofacial dysjunction, the midface or facial bones are separated from the cranium. Due to this fracture, the zygomaticofrontal suture is transverse, and is then continued through the floor of the orbit, and finally the nasofrontal suture. These fractures are usually asymmetric on both sides, and minimum mobility may be present.
Treatment depends on how badly the bone is broken. Surgery is preferred when the fracture is displaced and mobile. The benefits of the surgery include:
- Relieves pain
- Faster and better healing
- Supports the shape of the jaw and keeps your teeth in line that allows you to bite normally again
- Reduces the risk of infection and dental damage
- Improve speech and breathing pattern
- Improve ability to eat properly
What are the types of surgeries?
- Intermaxillary fixation (IMF)
It is a conventionally used procedure for the treatment of fractures that involve maxillomandibular complex. - Advanced techniques
The advanced treatment options include extended reduction techniques involving the rigid plate and screw fixation of the facial buttress. Bone grafts are also used to replace missing or comminuted bone.
Which individuals are eligible for the surgery?
The doctors usually wait for few days after the injury until the swelling subsides to decide whether the surgery is required.
The individual with the following conditions are suitable for the surgery.
- Difficulty in opening your mouth
- Ecchymosis (discoloration of the skin)
- Trauma
- Problem in the vision
- A sunken eyeball
- Facial numbness
- Unacceptable change in appearance
How should I prepare for the surgery?
Before the surgery, you need to follow certain precautions:
- Stop taking anticoagulants or anti-platelet agents such as aspirin as it increases the risk of bleeding
- Avoid taking substances that cause allergy
- Quit smoking and drinking
- Stop eating or drinking for six hours before your surgery
- Notify your surgeon if you have any illness like cold, cold sore, stomach or bowel upset
What will happen during the surgery?
Computerized tomographic scans and newly developed 3-dimensional reconstructions have helped in the diagnosis, classification and the preoperative planning of maxillary fractures. The aim of these fractures is to re-establish preinjury occlusion and the normal face projection. To reach this goal, the maxilla must be aligned and stabilized to provide support and contour to the midface.
Intermaxillary fixation (IMF)
The occlusion between the dental arches is established with intermaxillary fixation (IMF) or maxillomandibular fixation. This is one of the simplest and effective treatment options and if IMF treatment is given in early stages, it can eliminate the secondary deformities.
In this treatment, arch bars are secured to the upper and lower dental arches with individual wire ligatures around the teeth. This technique is an old procedure and is commonly used with other immobilization and stabilization techniques.
Advanced techniques
In this technique, fractures are opened and are put back together and held in place using small plates and screws. Then the surgeon stitches the gums using dissolvable stitches. During the surgery, temporary wires or braces or sometimes screws are placed around the teeth to fix elastic bands to them. This helps to guide your bite into the right position before and after surgery.
What is the aftercare of the surgery?
Do not worry if you feel severe pain and discomfort at the surgical site. It takes nearly 6 weeks for your jaw to heal completely. You need to follow certain precautions for better and early recovery. They include:
- Apply ice packs in the early postoperative site to minimize swelling.
- Avoid forceful nose blowing for three weeks
- Consume soft diet for 4 to 6 weeks starting with liquids for the first 3-4 days
- Perform exercises consistent of mouth opening and excursive movements
- Avoid smoking for at least 2-3 weeks
- Take pain medications to prevent pain as suggested by your surgeon
- Keep your mouth as clean as possible by rinsing with a mouthwash or warm salt water to prevent infections
The dissolvable stitches may take 2 weeks or more to disappear. The wires, metal braces or screws will be removed when the surgeon observes that the fracture has healed completely.
You need to seek care immediately if you;
- Have trouble breathing
- Feel that bones in your face move suddenly
- Bleeding from the surgical site, nose or ears
- Have loosened distractor attached to your head
What are the postsurgical considerations?
The risks of the surgery include:
- Bleeding from the cuts inside your mouth which can be resolved by applying pressure over the site for at least 10 minutes with a handkerchief or a swab.
- Infection
- Numbness on the top lip is a common postsurgical complication. It may take several weeks to disappear.
- Sometimes teeth adjacent to the fracture site may be damaged by the screws used.
- Nasal septum bowing with possible nasal obstruction
- Shortening of upper lip vertical length
- Latrogenic gingival/soft tissue pedicle injuries
- Avascular necrosis of the maxilla
- Dysfunction of the Temporomandibular joint
- Complications associated with prolonged hypotensive general anesthesia