Brachial Plexus Injuries
- What are brachial plexus injuries?
- Causes of a brachial plexus injury
- Types of brachial plexus injuries
- Treatment for a brachial plexus injury
- Which individuals are eligible for the surgery?
- How should I prepare for the surgery?
- What will happen during the surgery?
- What is the aftercare of the surgery?
- What are the risks of the surgery?
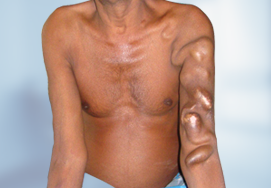
What are brachial plexus injuries?
The brachial plexus are the group of nerves that come from the spinal cord in the neck. These nerves control the movement and sensation in your hand, elbow, wrist, and shoulder. The radial, median, and ulnar nerves originate in the brachial plexus.
These nerves are injured due to stretching, pressure, or cutting. The nerve injury may lead to weakness, paralysis, loss of sensation. Some brachial plexus injuries are mild, and few are severe. Mild injuries recover spontaneously but may take several weeks to recover.
More severe injuries do not recover spontaneously and require surgery to regain function of the arm or hand and may cause permanent disability in the upper limb.
Causes of a brachial plexus injury
Brachial plexus injury (BPI) is an umbrella term for a variety of conditions that may impair function of the brachial plexus nerve network. The majority of pediatric and adult brachial plexus injuries are caused by trauma. The most common inciting events may include:
- Birth injuries – shoulder dystocia, forceps delivery
- High-speed vehicular accidents, especially motorcycle accidents
- Blunt trauma
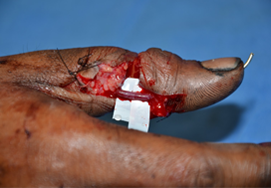
- Stab or gunshot wounds
- Inflammatory processes (brachial plexitis)
- Compression (for example caused by a growing tumor)
- Neuropathies
Types of brachial plexus injuries
Brachial plexus injuries are categorized according to the type of trauma experienced by the nerve. The following are the types of brachial plexus injuries:
- Avulsion – this means the nerve has been pulled out from the spinal cord and has no chance to recover.
- Rupture – this means the nerve has been stretched and at least partially torn, but not at the spinal cord.
- Neurapraxia – this means the nerve has been gently stretched or compressed but is still attached (not torn) and has excellent prognosis for rapid recovery
- Axonotemesis – this means the axons (equivalents of the copper filaments in an electric cable) have been severed. The prognosis is moderate.
- Neurotemesis – this means the entire nerve has been divided. The prognosis is very poor.
- Neuroma – this refers to a type of tumor that grows from a tangle of divided axons (nerve endings), which fail to regenerate. The prognosis will depend on what percentage of axons do regenerate.
Treatment for a brachial plexus injury
Due to the broad spectrum of brachial plexus injuries, it is difficult to estimate the rate of spontaneous recovery. The potential for spontaneous recovery depends on the type and severity of injury. Therefore, prognosis must be assessed for each patient individually based on the type and severity of their injury, and the progression of any spontaneous recovery that may be occurring.
Nonsurgical treatment options for brachial plexus injuries
Depending on the degree of severity, some nerve injuries are able to heal on their own. If this is not a viable option for a particular patient, a surgical option may be recommended by the surgeon. Physical rehabilitation therapy is always part of the recovery process for a brachial plexus injury.
Surgical treatment options for brachial plexus injuries
The degree of functional impairment and potential for recovery depend on the mechanism, type, complexity of the brachial plexus injury, and time from injury. The most important decision your surgeons will make is determining if and when surgical intervention should occur. Learn more about surgery for a brachial plexus injury.
Which individuals are eligible for the surgery?
Your surgeon decides whether you are a right candidate for surgery, but you should have realistic expectation to undergo the surgery.
You should undergo surgery if you have,
- Complete and partial paralysis not showing signs of recovery within 6 weeks of injury
How should I prepare for the surgery?
Before the surgery, you need to
- Take the medication as prescribed by your surgeon
- Stop taking anti-coagulants and blood thinners
- Quit alcohol and smoking
- Stop drinking and eating before the surgery
What will happen during the surgery?
The surgery differs based on the type, the extent of the injury. The aim of the surgery is to realign the damaged nerves and restore their function.
- Nerve grafting: Your surgeon will make an incision in the skin. Then a nerve is taken from the donor site(nerve from the leg or the arm). The damaged nerve segment is removed, and the nerve graft is placed and sewed to form a bridge between the damaged nerve endings.
- Nerve repair: This procedure is preferred for sharp cut injuries . It is a procedure in which the two torn edges of the nerve are reattached with sutures.
- Neurtoisation: here donor nerves are used to neurotise the plexus to regain function. As proximal nerve stumps are not viable for repair.
What is the aftercare of the surgery?
After the surgery, you need to follow certain instructions recommended by your surgeon for fast recovery. You should:.
- Take the pain medications prescribed by your surgeon
- Wear a sling to protect your arm
- Perform range of motion exercises suggested by your physical therapist
What are the risks of the surgery?
The risks and complications of the surgery include the following:
- Bleeding
- Wound infection
- Tingling and weakness to the upper extremity
- Failure to improve
- Hematoma
- Seroma